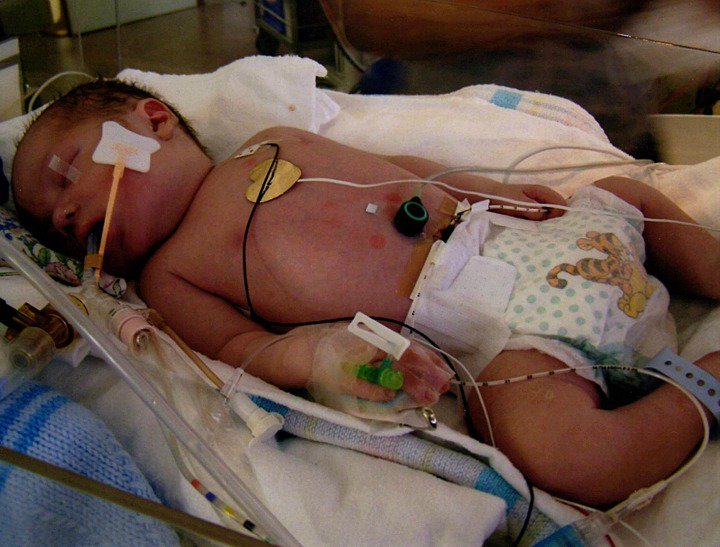
7.31 pm “We are going to lift your baby out slowly, so you may not hear him cry”.
Ok, so why isn’t anyone else in this delivery room making a sound either?
7.33 pm “He is having a little bit of trouble catching his breath, so we are going to take him to the nursery to give him some oxygen”
Is that why he is purple?
8 pm “It is getting late and your baby is still having a bit of a hard time with his breathing, we are thinking of transferring him to the hospital down the road as they can offer a higher level of care. Just in case…”
8.07 pm Seven minutes? Seven minutes ago you announced you were “thinking” of transferring my baby “just in case” and now here he is in a space age ambulance humidicrib with some kind of dome over his head and how did these people get here so fast and I’m starting to freak out and….
“What is your baby’s name?”
Joseph.
“My name is Anne. I promise you, I will look after Joseph”
Anne. The nurse with the black curly hair, the red rimmed glasses and the kind smile. Anne’s face is the image I cling to throughout the night as I drift in and out of exhausted sleep, punctuated by phone calls from the NICU at the hospital down the road…
“CPAP not working…Surfactant ….Meconium Aspiration….sediment…ventilator…oscillating respirator…”
Over the course of the next 10 hours and several phone calls only a few words managed to cut through the panic and exhaustion clouding my brain. As I fretted about my newborn baby boy with his purple skin and his bloated face, the panic started to rise up and threatened to overwhelm me. “He’s with Anne”, I would repeat over and over to bring myself back from the brink, and I would focus on the image of the nurse with the black curly hair, the red rimmed glasses and the kind smile.
As dawn finally broke the epidural had worn off enough for me to be transferred to the same hospital as my baby. After 4 days of gastro rampaging through my house like wildfire, taking my 2 ½ year old son, me, my husband and even my mum down with it, followed by 14 hours of labour and a rush in to theatre for an emergency caesarean, then the night of anguished torment I had just lived through, I was like the walking dead. Little did I know that I wasn’t emerging from Hell, I was still in it.
Hours before, I had been blissfully unaware of the existence of the Neonatal Intensive Care Unit. Even as we drove into the carpark of the Adelaide Women’s and Children’s Hospital I had no concept of this amazing hive of activity filled with the sound of beeping machines and the smell of hand sanitiser. A place where the air feels thicker, perhaps made so by the weight of the myriad of life and death decisions that are made there. A place where miracles happen daily but sadly, also a place where little angels often grow their wings.
The first time I saw Joseph in the NICU he was connected to a range of tubes, most importantly the one down his throat which was connected to the oscillating ventilator, a machine intended to shake loose the sediment of meconium that had settled like road tar in his lungs. Intellectually I know that to be its function, but witnessing it first hand was like watching some kind of torture device.
The image of my newborn baby son violently vibrating was so horrific that to this day it still provokes a physical reaction in me, causing the bile to rise in my throat. Where was Anne? I needed to see her to calm my escalating panic. Apparently Anne had finished her shift but here was Helen, another nurse with a kind face, reassuring me in her sing song voice with the strong Scottish lilt that Joseph was in good hands.
It was a few days before Joseph was declared stable, several more before they took him off the ventilator. Our experience in the NICU was a rollercoaster of conflicting emotions. We were so thankful he was alive and breathing (even with the assistance of the torture device), but wishing he was home with us, learning to breastfeed and keeping us up all hours of the night. I keenly felt a sense of loss – having experienced with my other son what the first few days with a newborn were supposed to be like – while also feeling guilty for feeling that way, when we were surrounded by so many tiny human beings clinging desperately to life. Friends were often afraid to call or send a card to celebrate his birth because we were all so unsure of what the outcome was going to be. In stark contrast were the NICU nurses, ready to celebrate every victory, no matter how tiny. In the world of the NICU, even a slight improvement in oxygen saturation levels had everyone cheering.
Throughout it all, the NICU nurses were there. There were so many who gave him such wonderful care but Anne and Helen remain in my heart. Anne not only helped me through that first harrowing night but she also allowed me my first cuddle with Joseph, 5 days after he was born. Helen spent many days and nights with Joseph and consulted us beforehand so that when decisions needed to be made in the middle of the night, she knew what our wishes were. She even left us a special note when Joseph “graduated” from the NICU to the Special Care Nursery.
Joseph spent 16 days in the NICU, another 7 days in the Special Care Nursery, and then came home on oxygen for the following 6 months. It felt like a lifetime. But at the same time, looking at our strong, energetic 7 year old, it also feels like a lifetime ago. The experience of Joseph’s birth has left scarring on his lungs, and we bear the emotional scars, but it has created a special place in our hearts for these amazing doctors and nurses who saved the life of our baby, and made possible all of the things he can do today.